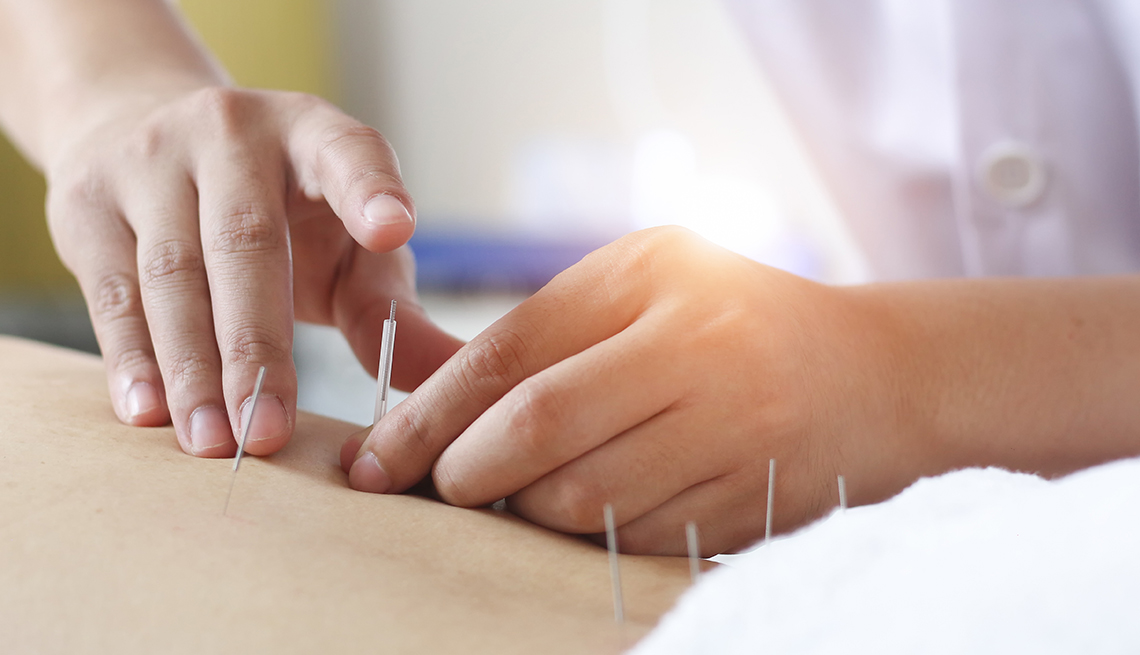
Acupuncture For Back Pain – By Acupuncture NYC Licensed Dr. Frank FengYu Zhao – Lower back pain is the top leading cause of job disability in the world, affecting about 80% of adults. Americans spend at least $50 billion per year on chronic back pain. The studies reveal that the medications and even surgery often fail to relieve the pain.
However, acupuncture is being recognized as a very effective therapy for lower back pain, especially it works for the patients who failed to get considerable relief from traditional treatments. A larger scale study conducted by researchers at Memorial Sloan-Kettering Cancer Center concluded that the benefits of real acupuncture are due to something more than the placebo effect. The effects of acupuncture are statistically significant and different from those of sham or placebo treatments. daftar slot
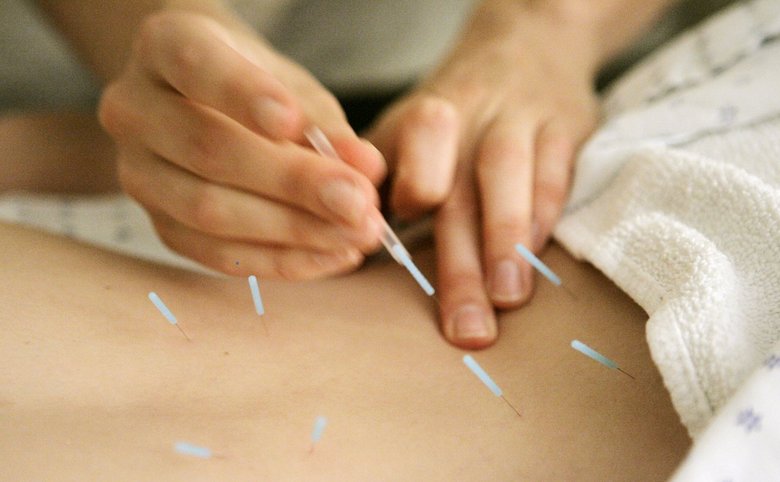
Another study conducted by researchers from the University of Maryland School of Medicine and the Peninsula Medical School, Plymouth, U.K. concluded that acupuncture is clearly effective in providing considerable true pain relief for people with chronic low back pain. Recent studies even demonstrated that acupuncture provides better effective for lower back pain than traditional medical treatments.
Why Acupuncture Appears better effective than traditional medical treatments for low Back Pain?
Pain is a distressing feeling often caused by intense or damaging stimuli, such as burning a finger, or broken the leg. Pain motivates the individual to withdraw from damaging situations, to protect a damaged body part while it heals, and to avoid similar experiences in the future.
Pain is usually transitory, lasting only until the noxious stimulus is removed or the underlying damage or pathology has healed, but it may persist despite the removal of the stimulus and obviously healing of the body.
Sometimes pain arises in the absence of any detectable stimulus, damage or disease. Because the chronic pain may arouse hyperalgesia in both peripheral and Central Nervous System.
Many factors such as genetic factor, social support, hypnotic suggestion, excitement, or distraction can significantly affect pain’s intensity or unpleasantness.
Clifford_J._Woolf suggests three classes of pains;
(1) nociceptive pain
(2) inflammatory pain which is associated with tissue damage and the infiltration of immune cells, and;
(3) pathological pain which is a disease state caused by damage to the nervous system or by its abnormal function (e.g. fibromyalgia, irritable bowel syndrome, tension type headache, etc.).
In 1968 Ronald Melzack and Kenneth Casey introduce a three dimensions conception of pain: “sensory- discriminative dimension” (sense of the intensity, location, quality and duration of the pain), ” affective-motivational dimension ” (unpleasantness and urge to escape the unpleasantness), just as definition of the pain: “pain is an unpleasant sensory and emotional experience associated with actual or potential tissue damage, or described in terms of such damage”, and “cognitive-evaluative dimension” (cognitions such as appraisal, cultural values, distraction and hypnotic suggestion).
They theorized that pain intensity (the sensory-discriminative dimension) and unpleasantness (the affective-motivational dimension) are not simply determined by the magnitude of the painful stimulus, but “higher” cognitive activities can influence perceived intensity and unpleasantness. Cognitive activities “may affect both sensory and affective experience or they may modify primarily the affective-motivational dimension.
Pain does not necessarily mean that something is damaged. But pain does mean that the brain is interpreting signals from the body that seem threatening. Sometimes those signals are amplified because of the superactivation of the pain pathways. And sometimes those signals are amplified because of the suppression natural pain-relieving pathways in the body. Whether you have over-activity of pain pathways or suppression of pain-relieving pathways or both, all these roads can lead to an increased sensitivity to pain.
The excitement in war or sports appears to block both dimensions of pain, while suggestion and placebos may modulate the affective-motivational dimension and leave the sensory-discriminative dimension relatively undisturbed.” Therefore, the Pain can be treated not only by trying to cut down the sensory input by anesthetic block, surgical intervention and but also by influencing the motivational-affective and cognitive factors as well.
Traditional medical treatments only treat the sensory-discriminative dimension while acupuncture can also adjust above three dimensions.
Acupuncture can trigger the release of natural opioid peptides in the brain that have an analgesic effect-natural pain-killer. There has been considerable evidence to support that acupuncture stimulates the central nervous system, releasing these opioid peptides.
Acupuncture can work on sensory- discriminative dimension and affective-motivational dimension. the patient often feels calm, relax and sleepy during the acupuncture treatment. Acupuncture can also Change brain chemistry by altering the release of neurotransmitters and neurohormones. Acupuncture is said to activate the hypothalamus and pituitary gland and thereby alter secretion of these chemicals. These particular chemicals play a direct role in the sensation of pain as well as the activity of an organ or organs.
Back pain is an aching feeling in the back, and can occur suddenly (like when lifting an object) or slowly progress with age. The intensity of back pain ranges from a sudden, acute pain to a chronic, mild pain to severe pain. Back pain can be the symptom of several different conditions, including a physical injury, herniated disk, kidney stones, pregnancy, scoliosis, arthritis and more.
Below you will find alternative and natural treatment options including those from a Chinese Medicine perspective for Back Pain.
Back Pain – Acupuncture Protocols
The treatment of conditions with acupuncture can be a complicated endeavor that should only be undertaken by individuals with a deep understanding of the theory of Traditional Chinese Medicine. There are many approaches, but generally speaking, few viable approaches are involved on a point to condition basis. Rather using proper diagnostic procedures the patients diagnostic patterns ascertained and that is what is treated.
The protocols listed here exemplify some of these clinical approaches.
The following Acupuncture Treatment Protocols May Be Used With Back Pain.
Below you will find some of the more common TCM diagnoses and acupuncture treatment protocols for low back pain and related issues. There are many ways to treat this condition with Eastern Medicine and our presentation is only one of many possible options.
Etiology & Pathology:
1. Stagnation of Qi and Blood in the lumbar region due to trauma (i.e. sprain or contusion).
2. Invasion and retention of pathogenic cold/wind/damp in the corresponding channels and collaterals (i.e. the Urinary Bladder, Gall Bladder and Governing Vessel Channels) causing obstruction and retardation of the circulation of Qi, and resulting in pain.
3. Deficiency of the Kidney Yin or Yang
Differentiation:
1.Stagnation of Qi and Blood
Signs & Symptoms:
1) History of Sprain, Trauma
2) Pain usually fixed and aggravated upon movement and/or pressure, needling or stabbing like pain, Pain and/or rigidity of lower back.
Treatment Points:
First, needle the remote Points, manipulate the needle with reducing method for 1-2 minutes and ask the patient move the back slowly. If the patient responds well, repeat this process a few times then insert local points and retain for 15-20 minutes.
Remote Points:
1) GV 26 – if pain is only in the midline of the back and patient has flexion/extension difficulty
2) SI 3 – if pain is in the posterior midline and also lateral and/or patient has torso rotation difficulty
3) Yaotongxue – if pain is on either side of the posterior midline, pain above UB 23.
4) UB 40 – acute back pain on the UB meridian, pain below UB 23. Let the patient stand, do micro bloodletting at UB 40, then do cupping to improve the effective of micro bloodletting.
5) LI 10 – stiff and/or rigid spine
6) GV 8 – stiff and/or rigid spine
2. Invasion and retention of pathogenic cold/wind/damp:
Signs & Symptoms:
1) The pain began after exposure to pathogenic cold/wind/damp. Severe pain and love warm at the back if caused mainly by the cold.
2) Heavy sensation and pain in the lumbar region if caused mainly by damp. The pain moving from place to place if caused mainly by the win.
3) Stiffness of the muscles with possible limitation of movement
4) Pain usually involves a larger area and also be in the buttocks and/or down the leg
5) Area may feel cold to the touch and/or to the patient
6) Pain is often weather related
7) Pain is not alleviated by bed rest
Treatment Points:
CV 4 – tonifies the yang and expels cold damp
GV 3 – expels cold damp
UB 23 – expels damp, tonifies the Kidney
UB 52 – chronic back pain above UB 23, direct needle towards pain
UB 32 – sacral pain
UB 54 – expels cold and damp
3. Kidney Deficiency:
Signs & Symptoms:
1) Pain is not severe – experience a sensation of soreness
2) Weakness in the lumbar area as well as in the knees
3) Fatigue and lassitude
4) Symptoms aggravated by exertion and alleviated by bed rest
5) Frequent urination, polyuria & other KD Qi Xu symptoms possible
Treatment Points:
UB 23, UB 52, GV 3, GV 4, KD 3 – strengthen the Kidney
UB 37 – history of trauma and stagnation of Qi and Blood
UB 57 – spasm of gastrocnemius or pain radiates to area
UB 58 – the function of movement is impaired and back/leg pain is not so severe – or when there are signs of retention of damp and stagnation of Qi and Blood.
UB 59 – severe pain and limitation of movement
UB 60 – chronic back pain, both lumbosacral and posterior leg pain
UB 62 – dropped the foot or back and leg pain with difficulty walking due to spasm in the channel.
GB 30 – sciatica and hip pain, bi syndrome of hip
GB 31 – dispels the wind, dispels cold/damp, used for pain in lateral thigh
GB 34 – back and leg pain with GB channel involvement
GB 39 – pain that radiates to the lower leg, frequently used for neck sprains.
Auriculotherapy:
Point: lumbar, Shen Men, kidney, Occipital, Subcortex